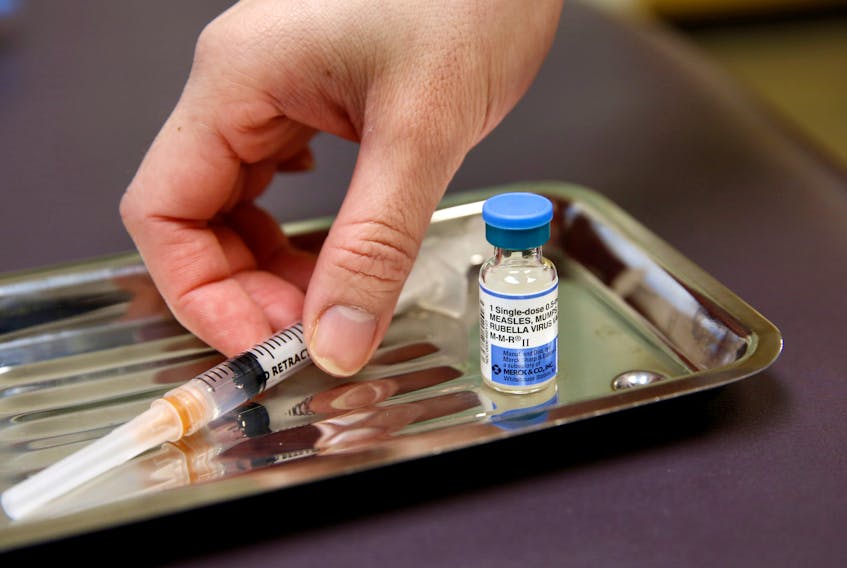
In 2000, measles was declared eradicated in the United States . But as of last week, 626 measles cases had been reported so far in 2019, a new record. That’s up from 327 cases in all of 2018, 120 in 2017 and 86 in 2016. As you can see, things are not going well.
The reasons for the resurgence of measles are manifold. Up until recently we were doing very well at vaccinating children in the developed world, but vaccination rates in the developing world have remained low. Worldwide, 20 million children miss out on the measles vaccine every year. So, measles persists in many countries and travellers to these countries can reintroduce the disease upon their return.
While it is tempting to consider measles a “minor” disease, it should be remembered that it does kill people. Even in the developed world, measles results in two to three deaths for every 1,000 cases . A serious complication like pneumonia occurs in 6-7 per cent of cases and measles encephalitis in another one case per thousand. The risk may seem small, and indeed it is, but prior to the introduction of vaccination, 300,000-400,000 Canadians would catch measles every year. If you do the math, you will see that this amounts to several hundred deaths.
But this article is not for the people who are reluctant to vaccinate. It’s for the people who want to protect themselves.
The other day I was asked what someone should do if they were concerned about contracting measles due to the recent uptick of cases. The obvious answer is to make sure one’s vaccines are up to date. The first measles vaccine was introduced in Canada in 1963, and widespread vaccination programs were introduced in the early 1970s. Anyone born before 1970 is usually assumed to have had measles as a child and to have become immune that way. In 1996, a second dose of the vaccine became part of the immunization schedule and anyone vaccinated after that time is also usually assumed to be immune.
Which raises the question of what to do with someone born after 1970, but who only received one dose of the vaccine. It is possible for immunity to wane with time. Someone who received only one dose of the vaccine 30-some-odd years ago may no longer be immune.
Measles is very contagious and a person can infect 90 per cent of their close contacts if those contacts are not protected. The people at greatest risk are those who travel to places where measles is still common and are not themselves immune. Military personnel (because they travel abroad) and health-care workers (because they come into close contact with infected persons) are also at higher risk. And finally, there are a few people who either cannot get the vaccine for medical reasons or who remain non-immune despite vaccination.
Unsurprisingly, protocols are in place to screen medical personnel to make sure they are immune to measles and other diseases. As a medical resident, I had to get checked for all my vaccines and needed to get a booster shot for measles. If there is any doubt about your immune status, this can easily be checked by measuring the level of IgG antibodies. If you are found to be non-immune and are at risk for measles, a booster may be a good idea. Specifically anyone who received a single dose of vaccine as a child may want to consider a second dose.
Some famous people have “concerns” about vaccines, but we would all likely be better off if we did not seek medical advice from movie stars, athletes and whatever an Instagram influencer is. The World Health Organization declared vaccine hesitancy one of the top 10 threats to global health in 2019. I would listen to them instead.
Christopher Labos is a Montreal doctor and an associate with the McGill Office for Science and Society. He also co-hosts a podcast called The Body of Evidence.
Copyright Postmedia Network Inc., 2019